What is Glaucoma?
Glaucoma is a leading cause of blindness. At least 3 million Americans suffer from glaucoma. Glaucoma is a disease of the optic nerve. The optic nerve is the cable that carries the information about the images we see from the eye to the brain. Many glaucoma cases are associated with elevation of eye pressure. Glaucoma optic nerve damage without high eye pressure is referred to as “low tension glaucoma” or “normal pressure glaucoma.” Glaucoma treatment, whether it is medication, laser, or surgery, aims to reduce eye pressure in order to protect the optic nerve and prevent vision loss.
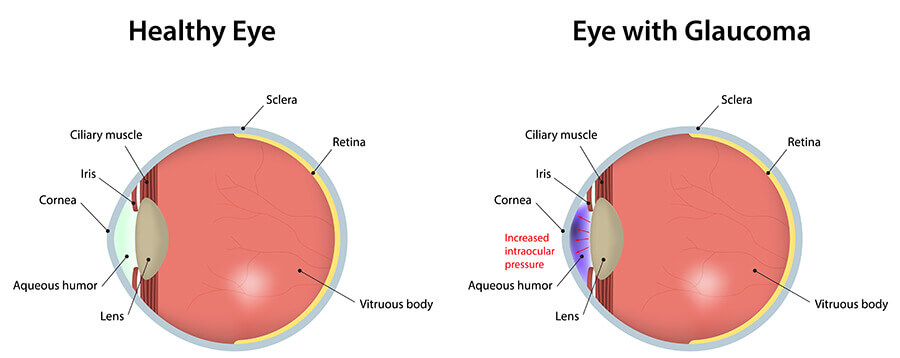
Visual loss from glaucoma results from damage to the optic nerve which leads to progressive loss of the field of vision. Usually people do not notice these blind areas until much of the optic nerve damage has already occurred. If the entire nerve is destroyed, blindness results. Early detection and treatment are the keys to preventing optic nerve damage and blindness from glaucoma.

Who is at risk for Glaucoma?
High eye pressure alone does not mean that you have glaucoma. A qualified ophthalmologist takes many kinds of information into account to determine your risk for developing the disease.
Several important risk factors include but are not limited to:
- Age
- African ancestry
- A family history of glaucoma
- Past injuries to the eyes
Your doctor will weigh all of these factors before deciding whether you need treatment for glaucoma or whether you should be monitored closely as a glaucoma suspect. If you are labeled as glaucoma suspect, it means that your risk of developing glaucoma is higher than normal and that you require more extensive monitoring.
Types of Glaucoma
Primary Open Angle Glaucoma
The vast majority of glaucoma patients have primary open angle glaucoma (POAG). The rise in eye pressure associated with open angle glaucoma has to do with a cell problem at the drain (trabecular meshwork) that increases resistance in the drain.
Closed Angle Glaucoma
This is a process in which the drain (trabecular meshwork) is blocked by the iris, leading to high pressure. Acute angle closure glaucoma is a medical emergency of high eye pressure that can lead to sudden and permanent blindness. This attack of glaucoma occurs when the drain is suddenly blocked, and is associated with severe eye pain, blurring of vision, colored halos around lights, nausea and vomiting. Chronic angle closure glaucoma occurs when scar tissue slowly clogs the drain and leads to high eye pressure and optic nerve damage.
Other Types of Glaucoma
There are other types of glaucoma, such as glaucoma associated with trauma or inflammation, pseudoexfoliative glaucoma, pigmentary glaucoma, or neovascular (new blood vessel) glaucoma. Congenital glaucoma refers to a glaucoma someone is born with and is associated with abnormal eye anatomy.
How is Glaucoma Detected?

Regular eye examinations are the best way to detect glaucoma. During a complete and painless eye exam for glaucoma, your doctor will:
- Check your vision
- Measure your intraocular pressure (tonometry)
- Examine the external anatomy of the eye
- Evaluate the optic nerve appearance (ophthalmoscopy)
If there is concern for glaucoma, additional testing may be performed. This can include:
- Gonioscopy (exam of the internal drains of the eye)
- Imaging of the optic nerve
- Visual field testing to detect peripheral (or side) vision loss
How often should a person with glaucoma see an ophthalmologist?
After the initial examination and diagnosis, glaucoma patients are managed like other patients with chronic disease, requiring regular visits to assess disease severity and response to therapy. Most patients will need periodic medical examinations, diagnostic testing and individualized management with drugs or procedures. Once the diagnosis and treatment regimen are established, the average patient needs to be seen 3-4 times yearly. Frequency of visits and testing depends upon risk of progressive damage and severity of glaucoma.
Eye drops for Glaucoma
If you are diagnosed with glaucoma, eye drops may be prescribed to control pressure in your eye. Eye drops lower eye pressure, either by decreasing the amount of fluid produced within the eye or by improving the drainage of fluid from the eye.
Glaucoma medications can preserve your vision, but they may also produce side effects. You should notify your ophthalmologist if you think you may be experiencing side effects.
Lasers Treatments
Laser treatment of Anatomical Narrow Angles or Angle Closure Glaucoma
Angle closure involves the lens coming too close to the iris and blocking the passage of fluid into the front of the eye. Relief of this block allows the iris to move away from the drain and the drainage angle to open, allowing escape of fluid and lowering of the eye pressure. This is now commonly and simply done by making a small hole in the iris with laser (laser iridotomy), which provides another route for fluid to enter the front of the eye. For additional information, ask your doctor about the laser iridotomy procedure.
Laser treatment of open angle Glaucoma
Laser trabeculoplasty is a simple office procedure that has gained wide acceptance in the treatment of open angle glaucoma. The newer laser surgical option for treatment of open-angle glaucoma is called selective laser trabeculoplasty, or S.L.T. During the S.L.T. procedure, your doctor directs a low frequency laser beam into the trabecular meshwork, which is the primary drainage region of the eye. The S.L.T. laser selectively treats specific cells leaving untreated portions of the trabecular meshwork intact. The procedure increases drainage of fluid out of the eye, resulting in lowered pressure in the eye. For more information, ask your doctor about the S.L.T. procedure.
Surgical Treatment of Glaucoma
There are many surgical options available to treat glaucoma. Filtering procedures have been developed to shunt the fluid from the inside of the eye to a reservoir under the conjunctiva on the surface of the eye to bring down eye pressure. Trabeculectomy is a common operation for the control of elevated intraocular pressure in adult glaucoma. Glaucoma drainage devices, such as the Ahmed valve or the Baerveldt drainage implant, are another excellent option to control eye pressure. Cataract surgery can help to lower eye pressure and has the benefit of improving vision at the same time. A variety of minimally invasive glaucoma surgeries may be performed as stand-alone procedures or in conjunction with cataract surgery to lower eye pressure. Research is ongoing and there are many novel and exciting glaucoma procedures. For more information about surgical treatment of glaucoma, and whether one of these procedures may be right for you, consult with your doctor.
Source: American Academy of Ophthalmology and American Glaucoma Society
Dr. Shayna Mangers is a fellowship trained glaucoma specialist and a member of the American Glaucoma Society. She will work with you to create a glaucoma treatment plan customized for you, taking into account your medical conditions, lifestyle, and personal preferences.
For more information, including frequently asked questions, please visit the American Glaucoma Society website.


